

Vitamin D and sleep
Hypothetical mechanism of action of vitamin D in sleep regulation
Although the exact mechanism of the effect of vitamin D on sleep regulation is still unclear, the presence of vitamin D receptors in brainstem areas involved in sleep regulation (anterior and posterior hypothalamus, black matter, midbrain grey matter, sutural nucleus, reticular nucleus) confirms its involvement in sleep regulation. Like other neuroactive steroids, vitamin D modulates neuronal excitability, action potential duration and neurotransmitter sensitivity, and affects neurotransmitter receptors such as the GABA and NMDA (N-methyl-D-aspartate) receptor, moreover, it affects the synthesis of many neurotrophins, and therefore has multiple effects on neuronal development, maintenance and survival [5]. Furthermore, there is evidence that vitamin D contributes to the regulation of the production of melatonin, the pineal gland hormone that controls the human diurnal rhythm and sleep. By acting on tryptophan hydroxylase (TPH)-2, vitamin D regulates the conversion of tryptophan to 5-hydroxytryptophan, which is metabolised to serotonin and then to melatonin [5].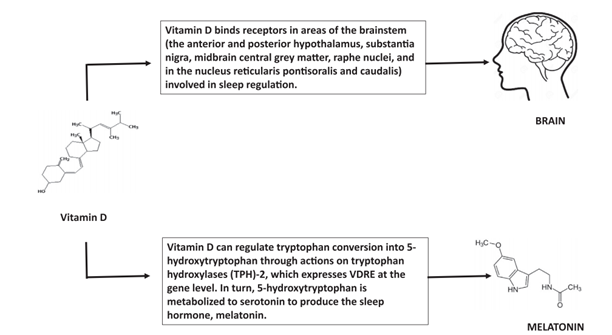
State of knowledge on vitamin D and sleep in healthy people
Ten observational studies and one intervention study were conducted to evaluate the effects of vitamin D levels on sleep in healthy people. Two observational studies on 800 Chinese adolescents (8-14 years) [6] and 1614 Korean older adults (60-80 years) [7] assessed the association between serum 25(OH)D concentration and sleep duration. Both studies showed a significant positive correlation between sleep duration and serum 25(OH)D concentration. Another observational study of 3048 men over the age of 68 years assessed the effects of fasting serum 25(OH)D concentrations, measured at the start of the study (morning of the first day of measurement), on sleep duration, sleep efficiency (i.e., percentage of sleep time relative to time spent in bed), and wake time after falling asleep for five consecutive days. The study also took into account other factors that may have influenced sleep disturbances, such as body weight, time of year, alcohol consumption and medication use. The study confirmed that low 25(OH)D levels were associated with shorter sleep duration, as well as reduced sleep efficiency. Waking time after falling asleep was not significantly correlated with vitamin D status [8]. Four studies evaluated the association between serum 25(OH)D levels and subjective sleep quality using the Pittsburgh Sleep Quality Index (PSQI). The first two studies were conducted with 92 [9] and 890 [10] pregnant women, the next two studies were conducted with 1472 Korean electronics manufacturing workers [11] and 512 Japanese women aged 35-79 years [12]. Only in the study conducted by Gunduz et al. [9] found no statistically significant association between serum 25(OH)D levels and sleep quality, the other three studies showed that poor sleep quality was more likely in vitamin D deficient subjects than in those with higher serum vitamin D levels. A comparison of serum vitamin D levels and PSQI components showed that mean scores for subjective sleep quality, sleep latency and sleep duration were significantly higher in participants with vitamin D deficiency, indicating that participants with vitamin D deficiency had poorer sleep quality. A recent study on the association between serum 25(OH)D levels and sleep conducted with 1045 healthy individuals in Germany aged 18-79 years (including 512 men) confirmed associations of serum 25(OH)D levels with nocturnal sleep duration and middle sleep time. However, no association was found between total sleep duration and nighttime sleep efficiency. Higher serum 25(OH)D concentrations were furthermore associated with shorter waking time between falling asleep and waking up in men, but slightly longer in women. Furthermore, serum 25(OH)D concentrations showed no significant association with subjective sleep quality and daytime sleepiness [13]. Although several studies have shown a positive association between serum 25(OH)D or vitamin D intake and sleep or mood, there are also studies revealing no effect on sleep. Contradictions in the results obtained may be due to methodological inconsistencies between studies, such as different protocols and types of intervention. In addition to the limitations mentioned earlier, it should be noted that many of the studies analysed essentially ignored two potentially important aspects, namely the timing of blood sampling and/or supplement intake.Summary
Many recent studies indicate that vitamin D has both a direct and indirect role in sleep regulation. Although vitamin D deficiency has been linked to sleep disorders, there is still no evidence to concretely support a role for vitamin D supplementation in the prevention or treatment of sleep disorders, so more intervention studies are needed to better clarify these aspects.References
- Patrick RP, Ames BN. FASEB J, 2015; 29:2207-2222
- Eyles DW, Burne THJ, McGrath JJ. Front Neuroendocrinol, 2013; 34:47-64
- Eyles DW, Smith S, Kinobe R, et al. J Chem Neuroanat. 2005;29:21-30.
- Huiberts LM, Smolders KCHJ. Sleep Med Rev. 2021;55:101379.
- Muscogiuri G, Barrea L, Scannapieco M, et al. Sleep Med. 2019;54:262-265.
- Gong QH, Li SX, Li H, et al. Nutrients. 2018;10:1013.
- Kim JH, Chang JH, Kim DY, et al. J Am Geriatr Soc. 2014;62:2327-32
- Massa J, Stone KL, Wei EK, et al. 2015;38:251-7.
- Gunduz S, Kosger H, Aldemir S, et al. Nutrients. 2017;9:340.
- Cheng TS, Loy SL, Cheung YB, et al. Nutrients. 2017 Mar 29;9(4):340
- Jung YS, Chae CH, Kim YO, et al. Ann Occup Environ Med. 2017;29:25.
- Nakamura K, Hui SP, Ukawa S, et al. Sleep Med. 2019;57:135-140.
- Dogan-Sander E, Willenberg A, Batmaz İ, et al. PLoS One. 2019;14(7):e0219318.
Nota biograficzna

Marlena Dudek-Makuch, PhD (Pharm.), MSc, has 20 years of professional experience in phytochemical and biological research, and scientific information (assistant professor at the Department of Pharmacognosy, Poznań University of Medical Sciences). She is an author of research and review papers on the isolation and identification of compounds of plant origin, and evaluation of their biological activity. Since 2015, she has been teaching a postgraduate course in “Herbs in practice and therapy”. She is currently a member of the Regulatory Department, R&D Division, at CHC. In her position, she is in charge of preparing expert reports (clinical, non-clinical) for medicinal products, clinical reports for OTC switches, clinical assessments of medical devices, pharmacovigilance activities for medical devices, and safety assessment of plant-based raw materials used in medicinal products, medical devices, and dietary supplements.
tel.: +48 61 625 27 00
fax: +48 61 625 27 01
office@chc.com.pl
bd@chc.com.pl
purchasing@chc.com.pl
rd@chc.com.pl
BDO: 000102401
Wysogotowo
ul. Batorowska 52
62-081 Przeźmierowo
POLAND
District Court for Poznań - Nowe Miasto and Wilda in Poznań, the 8th Commercial Division of the National Court
KRS 0000871229
NIP 781-00-41-371
Share capital: 36 100 000PLN
© Curtis Health Caps. All rights reserved.


